Summary of New Inhalable Tuberculosis Treatment Could Replace Months of Daily Pills:
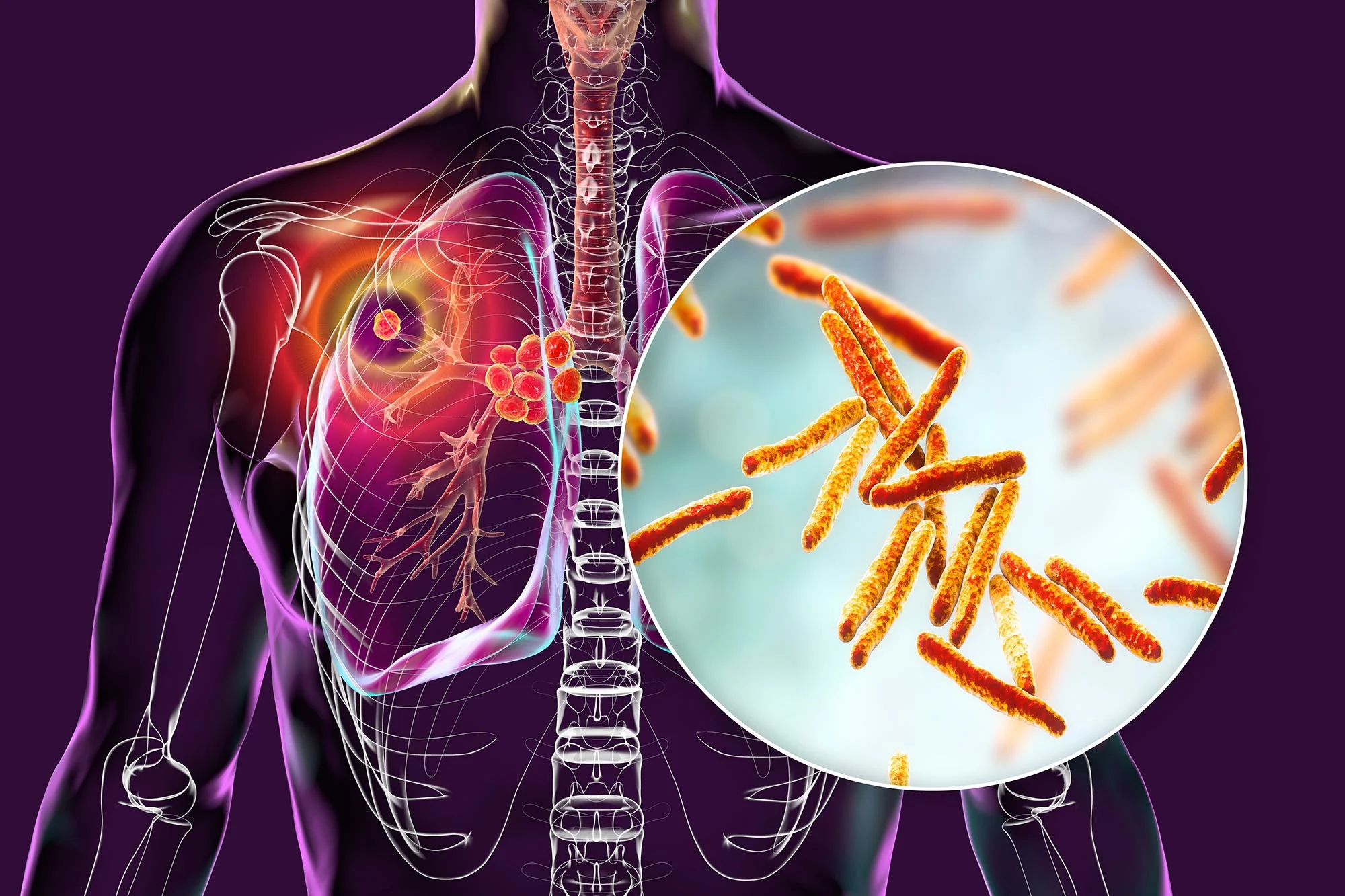
Researchers at the University at Buffalo have developed an inhalable nanoparticle system to deliver rifampin, a crucial tuberculosis (TB) drug, directly to the lungs. This innovative therapy aims to enhance treatment effectiveness while reducing side effects associated with oral dosing, as rifampin can harm the liver and has limited lung reach when taken as a pill.
The nanoparticle design uses biodegradable materials that adhere to immune cells called macrophages, allowing for prolonged presence in lung tissue and a potential shift from daily to weekly dosing. In mouse models, this approach significantly improved drug delivery to the lungs.
The research, published in Antimicrobial Agents and Chemotherapy, suggests that this system could simplify TB treatment, improve adherence, and reduce drug interactions with other medications. The next phase will explore combining this method with existing TB therapies. Beyond TB, inhalable rifampin could be beneficial for treating other serious lung infections.
*****
Summary Bullet Points
-
Inhalable Nanoparticle Therapy: Researchers at the University at Buffalo have developed an innovative inhalable treatment for tuberculosis (TB) that could significantly reduce the duration and frequency of medication.
-
Biocompatibility and Targeting: The nanoparticle system is designed to deliver rifampin directly to the lungs, enhancing its effectiveness while minimizing systemic side effects compared to traditional oral administration.
-
Improved Patient Compliance: With the potential to reduce treatment from daily pills to a less frequent once-a-week dosage, this research aims to enhance patient adherence, especially important for combating drug-resistant TB.
-
Broader Implications: Beyond just TB treatment, this inhalable therapy may address other serious lung infections and reduce harmful drug interactions, potentially leading to improved outcomes for patients with other pulmonary diseases.
- Future Research Directions: The next steps involve exploring how this nanoparticle system can work in synergy with other TB medications to establish a more effective treatment regimen.
An Innovative Approach to Tuberculosis Treatment
The world of medicine is constantly evolving, often taking leaps toward innovative solutions that can revolutionize how we approach some of humanity’s most challenging health issues. One such groundbreaking advance comes from the Jacobs School of Medicine and Biomedical Sciences at the University at Buffalo—a team of researchers has engineered an inhalable nanoparticle system crafted to transform the treatment of tuberculosis (TB). This development stands as a beacon of hope for millions affected by the disease, highlighting a promising future not only for TB treatment but for pharmaceutical interventions in general.
The Challenge of Tuberculosis
Tuberculosis remains one of the most insidious infectious diseases, claiming lives despite the existence of curative treatments. The conventional approach to TB therapy typically involves a demanding regimen of multiple oral medications taken daily for several months. This lengthy process brings with it a host of challenges, including severe side effects and the risk of treatment non-compliance—issues that can lead to treatment failure and the dangerous emergence of drug-resistant strains.
This is where the new inhalable nanoparticle system enters the picture. It’s not just a modification of existing treatment modalities; it’s a game changer that rethinks how we deliver life-saving medication directly where it’s needed most.
How It Works
At the heart of this innovative therapy is a specialized delivery mechanism designed to release rifampin, one of the most effective drugs for TB, directly into the lungs. Under normal circumstances, rifampin is administered orally, but only a fraction of the dose actual reaches the lungs, where the Mycobacterium tuberculosis bacteria reside. The new approach employs a biocompatible nanoparticle system, allowing the drug to be inhaled as tiny particles, crafted to optimize both delivery and effectiveness.
The scientists have designed these nanoparticles not merely as carriers but as intelligent agents that can communicate with the body’s immune system. These microscopic structures contain rifampin within a biodegradable core. They also feature an outer layer that targets macrophages—immune cells critically involved in the body’s defense against TB. As these nanoparticles are inhaled, they seamlessly attach to macrophages and release rifampin more effectively in the respiratory system, where it’s most needed.
The Benefits of Direct Delivery
Why is this method so groundbreaking? The inhalable treatment has the potential to keep rifampin in the lung tissue for extended periods, possibly requiring treatment just once a week instead of daily doses. Imagine the difference this could make in the lives of individuals grappling with the strict regimen of traditional TB therapy. The prospect of reduced dosing frequency could lead to higher rates of adherence, fundamentally transforming the TB treatment landscape.
Moreover, by delivering medication locally and effectively, this system mitigates some of the significant side effects associated with rifampin, such as liver damage. It allows for higher dosages where they are most effective without requiring the same measures of caution that oral delivery necessitates.
Research Findings
The researchers at the University at Buffalo conducted rigorous tests using mouse models that accurately reflect human TB infection. What they discovered was nothing short of remarkable: the inhaled nanoparticles not only kept higher concentrations of the drug in the lungs for much longer periods than traditional medication administration, but they also proved to be significantly more effective at reducing levels of Mycobacterium tuberculosis.
This isn’t simply a clinical achievement; it represents a pivotal moment in the scientific quest to better treat one of the world’s deadliest diseases. The study’s senior author, Dr. Jessica L. Reynolds, encapsulated the potential well: "Reducing treatment frequency could improve adherence, lower side effects, and make TB care more accessible worldwide."
Expanding Horizons: Beyond Tuberculosis
While the implications for TB treatment alone are extraordinary, the potential benefits of this delivering system extend far beyond. Rifampin isn’t limited to treating TB; it’s also effective against various serious lung infections caused by non-tuberculous mycobacteria, such as Mycobacterium kansasii and Mycobacterium xenopi. These infections pose significant challenges to individuals with chronic lung diseases, and the new approach could usher in an era of more effective treatment options for these patients.
Additionally, one cannot overlook the issue of drug-drug interactions that often arise when rifampin is taken orally. Due to its liver enzyme activation properties, rifampin’s effectiveness can be diminished when administered alongside other essential antibiotics, necessitating this approach’s further exploration. By directing the medication precisely where it’s required, this system opens the door for practitioners to utilize rifampin in situations it was previously avoided, vastly improving treatment regimens for patients with diverse pulmonary conditions.
Looking Ahead
The current findings represent but one chapter in a much larger narrative around the future of medical treatments for TB and beyond. The researchers have outlined their next steps: exploring the potential for combining this nanoparticle system with other standard TB treatments. Combination therapies continue to be a cornerstone of TB management, and enhancing their efficacy through such innovative delivery methods could potentiate even more effective treatment paradigms.
In a world where infectious diseases persist as global threats, innovative advances such as this offer not just scientific breakthroughs but also renewed hope. Patients grappling with the daily realities of chronic illness are often at the mercy of a healthcare system strung tight by resource limitations and complex therapeutic requirements. With each step toward better therapies, we inch closer to a world where such diseases can be managed more feasibly, enhancing both quality of life and treatment outcomes.
Conclusion
The advent of inhalable nanoparticle therapy signals a shift in how we conceptualize the treatment of complex diseases like tuberculosis. It invites us to rethink traditional methods and embrace innovative solutions geared toward improved patient experiences. Whether it’s the direct targeting of infected tissues, reduced side effects, or enhanced adherence to medication regimens, such advancements possess the power to significantly alter health landscapes.
In every trial and test, in every ounce of research and innovation, we move closer to an answer—a solution that not only treats the symptoms but also confronts the root of the issue. The quest for better health is continuous, and with each breakthrough, we are reminded of the resilience of science and the human spirit.
As you reflect on the complexities of health and disease treatment, consider how innovation can not only change lives but can also reframe the narratives around chronic diseases. It embodies a transformation that isn’t just scientific—it resonates deeply within the human experience, underscoring the power of hope, possibility, and relentless pursuit of improvement.